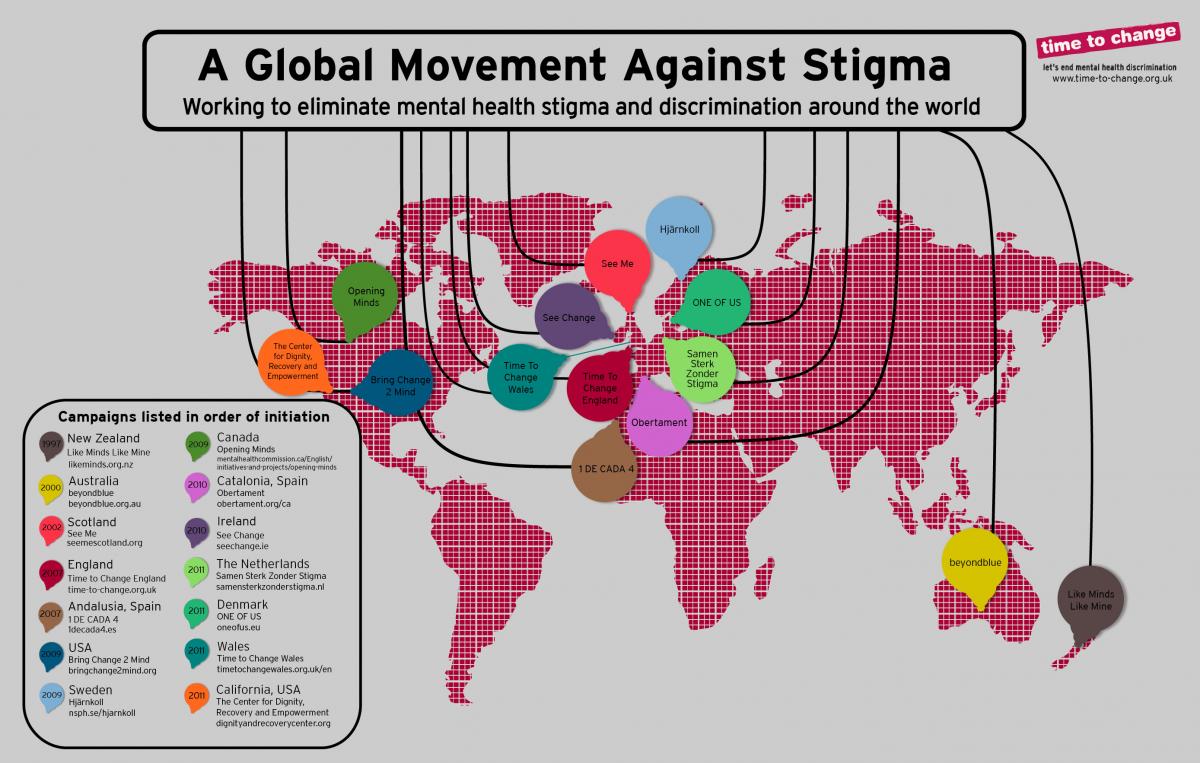
How anti-stigma campaigns are potentially making life worse - not better - for people in distress15/5/2019 Campaigns that raise awareness, normalise mental health difficulties and encourage people to tell their story enable the underlying sources of stigma to go unchallenged and the status quo to remain In recent years, public conversation around mental health has been dominated by the topic of stigma, defined as “a strong feeling of disapproval that most people in a society have about something, especially when this is unfair”. Other than occasional mentions of underfunding of services, stigma is the primary focus of the media and of campaigning efforts by charities. In these contexts, stigma is usually framed as incidences such as strangers hurling verbal abuse or workplace bullying.
There is no doubt that these kinds of interactions happen and that they can be hurtful and traumatic. I have experienced this from the public I encounter in my job and also A&E staff during a mental health assessment. I have met people who use residential mental health services who have been verbally abused by the neighbours that live nearby. However, I believe that this narrow focus on interpersonal stigma distracts from the underlying purveyors of stigma - mental health services and the medical model of distress. Before examining how these entities contribute to creating far more stigma than random bad eggs encountered out and about, we must first ask ourselves a question. Is this an intentional move, and if so who benefits and how?
1 Comment
Ofsted is changing the way it conducts inspections. Drawing on the views of students, we take the opportunity to think about how the education system could go from coercive to nourishing Christopher Bagley
In a previous blog, Psychologists for Social Change (PSC) responded to the announcement that the education regulator, Ofsted, are to update the framework they use to inspect schools in England. Having looked at the changes that Ofsted are proposing and finding them extremely narrow, the purpose of this article is to go further and envision an alternative future for the education system. It is based on PSC’s joint submission to the public consultation on Ofsted's proposals changes. When thinking about change in a democratic society, it is only right to begin by asking the people that will be directly affected. To this end, we spent time with States of Mind, a social enterprise that gives young people a platform to discuss issues related to education and mental health. Since January, States of Mind has conducted focus groups with 80 young people to elicit their views about the impact of Ofsted’s inspection framework on their education. Those involved were very keen to share their views: “We feel that our voices and experiences are constantly overlooked and neglected... we believe that it is our right to tell the true story of how the current system is failing us.” The students have written a powerful letter to the head of Ofsted, Amanda Spielman, communicating their deep concerns about the system’s negative impact on students. They also put forward psychological healthy ways of doing things differently. We draw on some of their ideas for this article. We also heard from parents and mined our own experience as teachers and educational psychologists. In austere times, outsourcing health services to private providers is becoming more common. To ensure service-users aren’t short changed and public spending isn’t wasted, commissioners need to take a much more hands-on approach Changing eating habits is often an element of a behaviour change programme
Recently, I spent a period working as a clinical psychologist in a health and well-being service, commissioned by a local authority in response to the UK’s obesity rate. The service is run by a small private organisation and was set up to promote healthy lifestyle behaviours. One of its aims is to support people to achieve a healthy weight to reduce the risk of preventable weight-related diseases and the human and economic costs associated with these. It does this with programmes designed to change people’s behaviours around food and eating and increase their physical activity. Aspects of the service were very encouraging. The team deployed creative ways of engaging local communities, statutory services and charities, ensuring a steady stream of suitable people referred to the service. It had established a strong presence in the community by taking part in health and wellbeing campaigns. The programmes were delivered by an enthusiastic though overstretched team that strongly abided by the “code” of the healthy lifestyle behaviours they promoted. A particularly exciting aspect of the service was that commissioners had recognised the role psychological and psychosocial factors play in the development and maintenance of obesity and behaviour change – hence the opening for a psychologist. I was excited to get stuck into my role, supporting this already vibrant service by integrating psychological theory and practice into the service delivery. Alas, my enthusiasm was short-lived. As I gained insights into how the service functioned, a nagging sense of unease took hold. A feeling, I now think, that stemmed from a tension created by the outsourcing of public services to private providers. It is hard to believe that the consequences of this tension are limited to this particular service - after all, in current economic times, this model of service procurement is becoming the norm. In fact, while writing this article, I had numerous conversations with colleagues working within the public and education sectors who found my experiences resonated with their own. This further convinced me to share my experiences as I hope they will stir up a further discussion. The UK government's ‘Prevent’ policy has put counter-terrorism on the agenda for social workers and health practitioners but what are the ethical implications for the services and the impact on the people they serve? Since the London tube bombings in 2005, counter-terrorism policy in the UK has extended into many areas of daily life. Introduced in 2006, the UK government’s Prevent strategy has put staff in areas such as local government, health and education on the front lines of domestic security and even border control, making them responsible for identifying and reporting those they consider at risk from ‘radicalisation’. The extension of counter-terrorism to the safeguarding of vulnerable individuals such as children is unique to Britain and the ethical dilemmas it poses for professionals who work with communities rendered suspect by Prevent are only beginning to be explored. In 2016 a UN special rapporteur criticised Prevent on grounds that the government’s definition of domestic extremism was too broad, noting concerns about “the program being implemented in a way that translates simply into crude racial, ideological, cultural and religious profiling, with consequent effects on the right to freedom of association of some groups.” Muslim groups and charities including Amnesty International and the Muslim Council of Britain have raised concerns that the policy creates division and resentment. Anxieties about terrorism can lead to a climate of fear in which vaguely defined ‘security risks’ can become pretexts for political repression, greater government intervention in daily life and even deprivation of the rights and protections afforded by citizenship. The introduction of pre-emptive ‘risk work’, analogous to duties performed by the security services, into health and social care settings may adversely impact communication between service users and professionals and deter help-seeking – especially in scenarios where children may be removed from their parents' care. Researchers in health and social care have begun to assess the implementation of Prevent to ask whether Muslim groups are right to see the policy as discriminatory. Questions include the impact of pre-existing biases among professionals on referrals and over the validity of the ‘conveyor belt’ model of radicalisation – a key premise of the policy which places 'moderate' religious and political beliefs and behaviours on a continuum leading to 'extreme' beliefs and potentially violent acts. On 22nd January 2019 the government announced an independent review of the Prevent strategy, raising the possibility that the policy may be reformed. However, security minister Ben Wallace has sounded a defensive note, demanding "solid evidence" that Prevent is in fact discriminatory and accusing the policy’s critics of using "distortion and spin" to raise concerns over its effects. In such a highly contested and politicised area, concerns about national security are sometimes invoked in a way that shuts down debate. Is it possible for health and social care professionals to stand in solidarity with service users who feel victimised in this climate? Given that Prevent remains a statutory duty as part of safeguarding, how can professionals think through the ethical and professional dilemmas it raises when working with families from communities that feel unfairly targeted? Even if the policy ends, what can we learn from the issues and debates prompted by its implementation? If you are a health or social care professional interested in knowing more, come to the joint BASW (British Association of Social Workers) London and MedAct event on Thursday 21st March. Advocacy groups, social workers and academics will present some of their findings on the above topics and MedAct will facilitate a discussion and workshop: https://www.eventbrite.co.uk/e/the-impact-of-the-prevent-policy-on-children-and-families-tickets-57231284312 Why the proposed changes to the Ofsted inspection framework won’t deliver and what we need to do to really benefit our children and young people Christopher Bagley
In December 2017, the UK Government released a Green Paper entitled Transforming Children and Young People’s Mental Health Provision. In response, Psychologists for Social Change wrote an open letter, signed by 1400 psychologists, teachers, social workers, students and counsellors, as well as young people with lived experience of mental health issues and their parents. In it, we urged the government to “take a genuinely preventative approach” to mental ill-health, by acknowledging and addressing the wider social factors known to be linked to distress, as well as bringing an end to the austerity policies that have exacerbated these. You can read our review of the finalised proposals, published this summer, here. In short, we believe they fall desperately short of addressing the underlying barriers to long-term improvements to our collective mental health. We also called on the government to review the toll that accountability measures like exams and ‘teaching to the test’ are creating, which, according to the National Education Union, are a great source of emotional distress for teachers and pupils alike. Currently, Ofsted holds teachers and schools accountable for the academic results of young people. Every child is expected to achieve a pre-defined, government set ‘standard’. Anything else is viewed as failure for the school, regardless of a young person’s needs or the pupil demographics of the area. This leads to teachers spending hours assessing students, tracking and logging data. Workload stress is having an increasingly detrimental impact on the mental health and job satisfaction of teachers. Schools can struggle to retain teachers. In short, things are bad before we’ve even considered the impact on students. For them, the focus on results means an inflexible curriculum, with limited opportunity for creativity and a narrow conception of what intelligence and achievement means. For those who struggle to make progress, constant messages about not achieving ‘expected progress’ can be catastrophic to their mental health. Loneliness, like so many things in post-austerity Britain, has became all about productivity and profitability Ruth Cain
Only some of this is true, but it is true enough. I am divorced and live alone in London, a city of 10 million people, around one third of whom live alone. There are four or five people I would consider ‘real’, long-term friends. They are mostly spread across the country and indeed the world, from Durham to New Zealand. Although some friends tell me that I can always talk to them, there is no one who I would automatically feel able or entitled to call in a crisis. This makes me one of the two-thirds of people in the UK who reportedly feel they have no one to turn to if in need. I work largely at home and so can spend several days not talking to anyone face to face, except the staff in my local supermarket or café. I spend a lot of time on screens, both for work and leisure, and have recently tried to cut down on social media as it is making me feel inadequate. Still, if I get rid of it, I will feel more cut off. I am not shy but the more time I spend alone, the harder it is to go out and talk to anyone, and the more anxious I become when talking to strangers or in groups. Recently, my instinct has been to turn down invitations. This profile puts me squarely into a box of people who the government have deemed likely to be lonely, based on research into the characteristics and circumstances of lonely people. I’m not alone in this box: according to the charity Relate, almost a fifth of adults feel lonely often or all the time. You could say that I’m part of the zeitgeist. Loneliness is hot right now – both in the halls of Westminster and around the kidney-shaped tables of start-ups, incentivised to make a buck out of our unwanted solitude. On Valentine’s day, the BBC launched a loneliness survey and 55,000 people from around the world participated, making it the largest ever survey into the subject. The results were turned into a series of three radio documentaries that aired in October. I’ve lost track of the number of articles I’ve read this year about a woman (because they usually are women) who moved to London and felt achingly alone in the middle of one of the busiest metropolises on Earth. It seems like we’ve been given permission to talk and the floodgates have opened. The continued attack on the welfare state under this government is being held up to international scrutiny and demands a response from psychologists PSC welcome the report by Philip Alston, United Nations Special Rapporteur on Extreme Poverty and Human Rights, on his visit to the United Kingdom. Although issues of causality are complex, there is significant evidence on the relationship between poverty, inequality and mental health difficulties. This report highlights the suffering that has been inflicted through the callous approach to austerity taken by the government since 2009.
It also recognises and gives voice to the impact that Universal Credit is having on people’s mental health, finances and work prospects. The continued attack on the welfare state under this government is being held up to international scrutiny and demands a response from psychologists. Many professions have been drawn into pushing the austerity agenda, including psychologists. It is important to recognise ours' and others' roles, including psychology’s continuing contribution to exploitation and oppression in the form of ‘enhanced interrogation’ and workfare. However, this report gives a firm foundation to organise around. In particular: 1) Austerity is not over and we still need to highlight it's pernicious effects 2) Universal Credit should be scrapped and we need to work with activists towards this goal 3) The continued cuts to local authorities are eroding a sense of community. Psychologists and others in positions of power working, purportedly, alongside those with less power, need to reach out to other professionals and activists and continue to work towards a just future that fulfils our commitments to truly promoting mental health and well-being. Concerned about the number of children living in squalid conditions in temporary accommodation, Jane Williams decided to do something about it. A year on, she has some learning to share with service providers Photo: Teri Pengilley for the Guardian
Jane Williams Tonight A will attempt to get a good night’s sleep sharing a double bed with her 18-month-old twins and her grandmother F will watch her 2-year-old daughter, already traumatised by domestic violence, kept awake and cowering by the shouts of drug users and drunks outside her door in B&B accommodation L will listen to her 3-year-old wheezing again because the window by her bed is cracked and mould on the wall is growing faster than she can clean it off. The doctor wants to charge £65 to write a letter confirming that her wheezing is made worse by the poor housing *** In December 2017, there were 1,994 under-fives living in temporary accommodation in the London borough of Newham. This number represents a need that is never-ending. It is refreshed weekly with the churn of new families being housed in Newham while others are moved away. I am able to give you a number thanks to a FOI request made by a newspaper. I’m not sure what the most up to date figure is as there is no agency that keeps track of the under-fives swilling from borough to borough, effectively homeless. I imagine it is likely to be about the same. Social disadvantage and inequality tug at the very fabric of what makes society functional. It is time to reflect this in our conversation about mental ill health First published on 20/5/2018 by The Independent during Mental Health Awareness week. Republished here on World Mental Health Day (Photo by Tom Parsons on Unsplash)
Annabel Head and Jessica Bond In 2018, mental health and psychological distress are high on the agenda. And this is great progress. The increased awareness of mental health issues and the willingness to discuss them that we are currently seeing is vital. It keeps pressure on policymakers to fulfil their promise to put mental health on an equal footing with physical health. To really make a difference, though, we need to take the conversation to the next level – to raise a different kind of awareness that leads to a different kind of action. Awareness about the root causes of psychological distress. We need to spread the message that the society and communities we live in and the way they are organised by social, political and economic forces play a significant role in our wellbeing. We need that message to become part of the conversation around mental health so that the ideas are built into the heart of all of our society’s policies, not viewed as only relevant to NHS mental health services. The case for the role that social, economic and environmental factors play in mental health and distress is robust. Psychological distress (often categorised as “mental disorders” and other terms we, as psychologists, are not always comfortable with) is not distributed equally across society. People lower down the socioeconomic ladder suffer more mental distress than those higher up, with the gradient particularly pronounced for women. Inequality is also associated with poorer wellbeing for those at the sharp end. Multiple studies have shown a link between low socioeconomic position and increased rates of depression and anxiety. Debt and having a poor-quality job – such as those with zero-hour contracts or where there is little control or reward to be had – are risk factors for experiencing distress. Unemployment is associated with a higher risk of suicide. Similarly, poor quality or overcrowded housing is linked to poorer mental health in adults and is worse for children’s educational and health outcomes. Living in a neighbourhood blighted by violence or with a high crime rate is associated with trauma. Those experiencing oppression through living in communities in which there are high levels of racial inequality and discrimination are more likely to feel distressed. Psychologists and social workers who see risk rather than need are doing families living in poverty a disservice Photo by Emma Goldsmith on Unsplash
Sinead Peacock-Brennan On August 16, the British Association for Social Workers (BASW) and Psychologists for Social Change (PSC) co-hosted an event to highlight social injustice and inequalities within the child protection and care systems. I work as a clinical psychologist in a service for people with a learning disability and have been an active member of London PSC for three years. At the event, the audience heard presentations based on research and practical experience of psychologists, social workers and people with lived experience of the care system. I agreed to summarise the points that resonated with me, along with some of my own thoughts. After the main presentations small groups discussed what they had heard and came together to think about individual and collective action. I've collated our ideas in part 2 of this blog: "We need to be more 'counter', committed and personal". You can read BASW's Eve Wilson's take on the event here and watch a recording of part of the event here. What does the research say? Professor Anna Gupta discussed her research, alongside that of Paul Bywaters, Andy Bilson and Michal Krumer-Nevo. Professor Gupta explained that a child is ten times more likely to be taken into care if they come from an area of high deprivation compared to an area of low deprivation. (Deprivation refers to a community's access, or lack of access, to important resources such as income, education, employment or health). This is also the case for children on a child protection plan, which is drawn up by the local authority and the family after an investigation to keep a child safe or improve their living conditions. As local authorities have continued to be hit by austerity, there has been an increase in the numbers of children on protection plans, most often for emotional abuse or neglect (the proportion of children in care for physical or sexual abuse appears to stay the same). Despite this increase, a large proportion of children are not being offered any service after the investigation. So, families are labelled as not providing “good enough” care but not “bad enough” to warrant support, a situation that Professor Gupta suggested has contributed to the relationship between services and families feeling increasingly authoritarian and coercive. What then is driving these differences in the involvement of child protection services? There is no evidence to suggest that parents in Blackpool (an area of high deprivation) love their children any less than parents in Wokingham (low deprivation). Is it down to the differing levels of deprivation? Professor Gupta talked about the direct and indirect impacts of poverty on children and families – both of which play a role. A direct impact would be the inability to buy food for your family if you do not have access to money. An indirect impact would be the lack of power that people living in poverty hold, blocking their access to roles, rights and opportunities as well as having an impact on the way professionals interact with them. |
AuthorPSC is a network of people interested in applying psychology to generate social and political action. You don't have to be a member of PSC to contribute to the blog Archives
February 2022
Categories
All
|
PSYCHOLOGISTS FOR SOCIAL CHANGE
- Home
- About
-
Groups
- Blog
-
Position statements
- UK >
-
Cymru / Wales
>
- Housing Support Funding
- Connecting the Dots Report
- Chemical Imbalance Myth
- Review of use of dx PD
- UK Inhumane Removal Plans
- WG LGBT+actionplan
- Ty Coryton
- Commission on Race and Ethnic Disparities: The Report
- ECT Review
- Black Lives Matter
- COVID 19 and Internet Access
- Save the T4CYP Programme
- Support the Mind over matter Report
- UN Report on Extreme Poverty in the UK Letter
- England >
- Ireland >
- Northern Ireland
- Scotland
-
Campaigns
- Join our mailing list








 RSS Feed
RSS Feed
